
What Is Macular Degeneration?
Macular degeneration, also called AMD or age-related macular degeneration, occurs when the macula — the central portion of the retina — begins to wear down, causing central vision loss.
People who suffer from AMD tend to lose their “straight ahead” vision, making it difficult to read, drive, and recognize faces.
Total vision loss is unlikely, as there's typically enough peripheral vision to allow for other activities of daily life.
Types of Macular Degeneration:
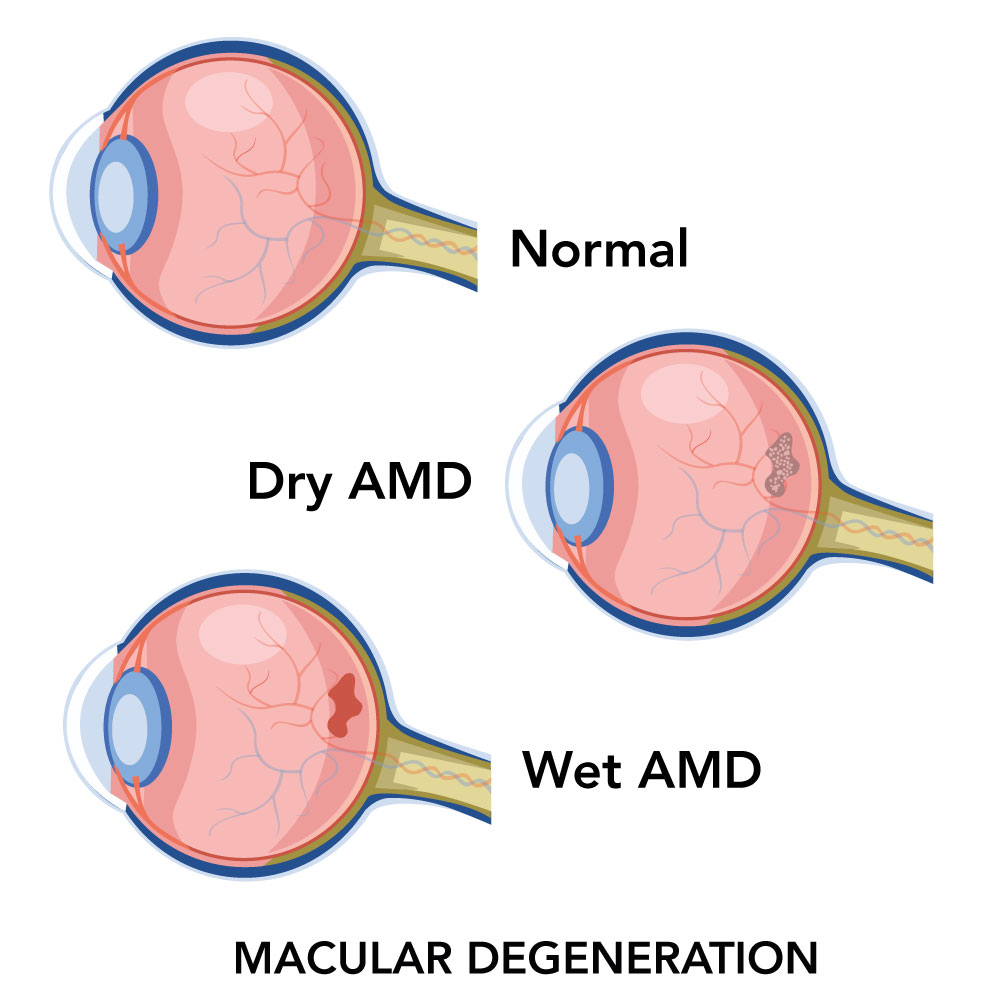
- Dry AMD: small deposits called drusen damage retinal nerve cells and reduce vision
- Wet AMD: new blood vessels form that leak and release fluid that harms the macula. This is a more severe form of AMD that can more quickly cause vision loss.
Don’t Let AMD Rob You of Your Sight
An estimated 196 million people are living with macular degeneration worldwide. Although those affected by it rarely lose all their vision, the vast majority suffer from some degree of vision loss.
While there is currently no cure for AMD, there are certain treatments that can slow its progression — and low vision aids that can increase independent functioning.
If you think you're at risk or are experiencing symptoms, contact Clear View Vision Care today. We can diagnose and help treat the disease.
Risk Factors for AMD
-
Aged 50+
The onset of AMD usually happens over the age of 50 and increases substantially with time. For instance, a 2% risk at age 55 can turn into a 30% risk by age 75.
-
Lifestyle factors
Smoking or eating a diet high in saturated fat can increase your risk of AMD. Furthermore, these habits increase the risk of high blood pressure and cardiovascular disease–two additional risk factors for AMD.
-
Obesity
Research shows that people with a BMI of over 30 double their chances of developing AMD.
-
Family History
If you have a close relative with AMD, you have a higher risk of developing this eye condition.
How to Stop the Progression of Macular Degeneration
While there isn’t yet a cure for AMD or an effective way of reversing vision loss that has already occurred, you can take certain steps and adopt new habits to slow the progression of the disease.
Furthermore, certain treatments can slow its progression and low vision aids that can increase independent functioning.
Talk to us about how you can slow the progression of the disease and avoid vision loss by contacting Clear View Vision Care today.

Macular Degeneration FAQs
You may have AMD and not know it. Typically, symptoms may not develop until the advanced stage of the eye disease.
First signs of AMD may include:
- Blurred vision
- Blind spots or dark spots
- Straight lines appearing distorted or wavy
- Faded colors
For early detection and better outcomes, it's important to undergo regular eye exams at our eye clinic, especially if you have a family history of AMD or other risk factors.
Statistics indicate that 8.7% of the world population has macular degeneration. The rate of AMD is expected to increase from 196 million in 2022 to 288 million by 2040.
Currently, the most common treatment for wet AMD is the injection of medications called anti-VEGF agents. High levels of VEGF in the eye increase the formation of abnormal blood vessels that cause much of the damage in wet AMD.
Macular Degeneration Treatment in Tucson

Meet our Eye Doctors

- Monday 8:30 am - 5:30 pm
- Tuesday 8:30 am - 5:30 pm
- Wednesday 8:30 am - 5:30 pm
- Thursday 8:30 am - 5:30 pm
- Friday 8:30 am - 5:30 pm
- Saturday Closed
- Sunday Closed
- VSP
- Medicare
- United Healthcare
- Aetna
- Cigna
- Spectera
- Superior Vision
- Davis Vision
- Tricare
- EyeMed
- Anthem Blue Cross Blue Shield
- Blue Cross
- MetLife

